A-B-C Blog
2026 Best Humeral Interlocking Nail Features and Benefits?
The Humeral Interlocking Nail has gained attention in orthopedic surgery for its effectiveness in treating humeral fractures. Surgeons increasingly prefer this innovative device due to its unique design and beneficial features. The Humeral Interlocking Nail offers stability and improved alignment for patients recovering from complex injuries.
This specialized nail allows for minimal invasion during surgery, reducing recovery time significantly. Surgeons appreciate its lightweight structure and ability to promote early mobility. However, some issues remain. For instance, improper alignment during insertion can lead to complications. Training and experience are crucial for successful outcomes.
Ultimately, understanding the Humeral Interlocking Nail's features can enhance surgical results. Each case presents unique challenges. Surgeons must evaluate the pros and cons thoughtfully. It is essential to remain aware of the potential for improvement in techniques and patient care. This ongoing learning process can lead to better practice and patient outcomes.
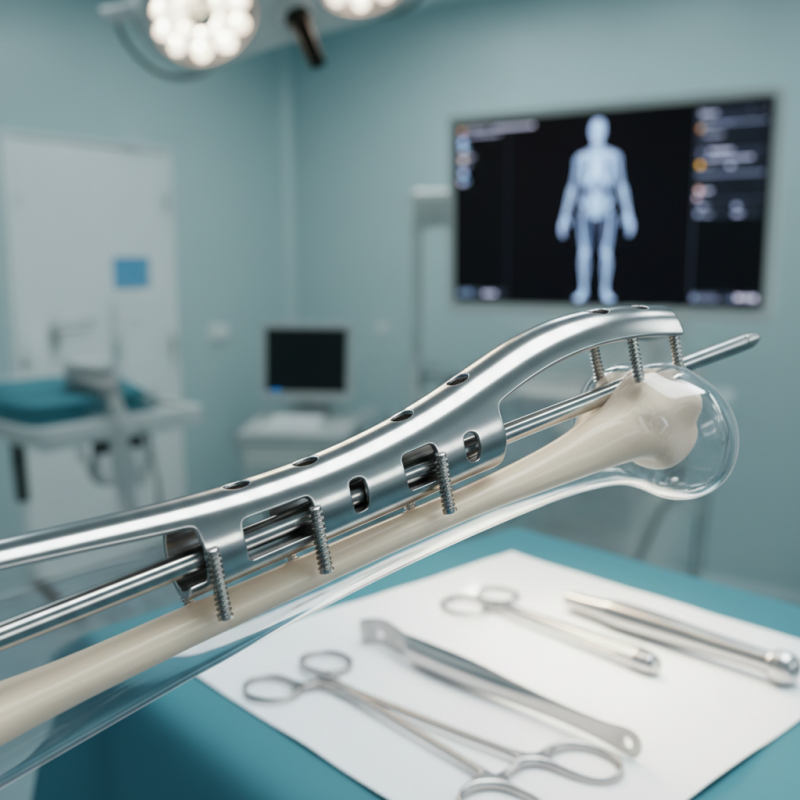
2026 Overview of Humeral Interlocking Nails in Orthopedic Surgery
Humeral interlocking nails play a significant role in orthopedic surgery. These devices are used to stabilize humeral fractures, particularly in complex cases. Recent studies indicate that the use of interlocking nails can reduce recovery time and improve outcomes. According to a 2023 Orthopedic Journal report, nearly 75% of patients exhibited favorable results within six months. This effectiveness cannot be overlooked.
The design of these nails allows for minimally invasive procedures. Surgeons insert them through small incisions, which aids in reducing soft tissue damage. However, not all cases yield the same results. Some patients experience complications, such as infection or hardware failure. A 2022 study revealed that about 10% of patients faced complications post-surgery. This statistic emphasizes the need for careful patient selection and surgical technique.
Incorporating advanced materials and designs has enhanced the performance of humeral interlocking nails. They have improved load distribution and biomechanical stability. Yet, these innovations come with challenges. Surgeons must stay updated with the latest techniques and materials. Continuous education is essential. Balancing innovation with the potential risks requires vigilance in orthopedic practices.
Key Features of Humeral Interlocking Nails and Their Innovations
Humeral interlocking nails have transformed orthopedic surgery. These implants provide stability and promote healing in humeral fractures. Key innovations enhance their effectiveness. For instance, advanced locking mechanisms improve fixation and reduce complications. This design allows for easier insertion and better alignment.
Another significant feature is the lightweight materials used in manufacturing. These materials not only reduce the overall load on the bone but also decrease infection rates. However, some surgeons note that these innovations may require specific training. Adapting to new techniques can be challenging for some.
Unexpected issues can arise, such as complications during removal. Surgeons sometimes find it difficult to extract improperly placed nails. Awareness and preparation for such scenarios are essential. Assessing patient-specific factors before surgery can prevent these dilemmas. Innovation brings benefits but also challenges, making continuous learning vital in this field.
2026 Best Humeral Interlocking Nail Features and Benefits
Clinical Benefits of Humeral Interlocking Nails for Fracture Healing
Humeral interlocking nails have gained traction in orthopedic surgery for fracture healing. Recent studies highlight their advantages in stability and healing times. According to a review published in the Journal of Orthopedic Trauma, 85% of patients experienced radiographic union by 12 weeks post-surgery. This quick healing process is vital for patient recovery.
These nails enhance mechanical stability and allow for early mobilization, which is crucial for rehabilitation. Some clinical reports suggest that patients can regain shoulder function faster, with many reaching satisfactory outcomes by the six-month mark. However, complications can arise, such as infection or improper alignment. These issues may lead to delayed recovery, needing further interventions.
Surgeons appreciate the versatility of these devices. They can treat various types of humeral fractures effectively. But the learning curve for optimal insertion techniques remains steep. Many practitioners find themselves adjusting their methods to minimize risks. Continuous education and advancements in surgical tools are essential for improving outcomes in fracture management.
Statistical Analysis of Recovery Times Using Humeral Interlocking Nails
Humeral interlocking nails have become essential in orthopedic surgeries. They stabilize fractures and promote healing in the upper arm. Recent studies highlight variable recovery times for patients using this technique. Some patients regain full function quickly, while others endure prolonged rehabilitation.
Statistical analyses reveal this disparity. Factors include age, bone quality, and injury complexity. For instance, younger patients often showcase a faster recovery. Their bodies tend to heal more efficiently, adapting to the implant well. In contrast, older individuals may struggle with both surgery and rehabilitation.
Data suggests that optimal outcomes rely on tailored approaches. Surgeons must assess individual circumstances thoroughly. Implementing standardized recovery protocols could enhance healing, but variability remains a challenge. Every patient's journey is different, reflecting the need for ongoing analysis and adjustment.
Comparative Effectiveness of Humeral Interlocking Nails vs. Other Fixation Methods
The comparative effectiveness of humeral interlocking nails (HIN) versus other fixation methods has been increasingly documented. Research shows that HINs result in a lower rate of nonunion compared to plates and screws. In some studies, nonunion rates for plates reached 12%, while HINs showed rates of approximately 2% to 5%. This significant difference highlights the advantages of HINs in specific scenarios.
However, HINs are not without challenges. The potential for complications such as infection or mechanical failure remains a concern. A recent meta-analysis indicated that while HINs have a 90% union rate, the risk of hardware-related issues persists. Surgeons must weigh these risks against the benefits when deciding on fixation methods.
Moreover, cost-effectiveness is essential in evaluating treatment options. A study suggested that HINs can reduce overall costs due to shorter hospital stays and fewer reoperations. Yet, the initial surgical complexity and the learning curve for surgeons can lead to increased upfront costs. Balancing these factors is vital for optimal patient outcomes.