A-B-C Blog
2026 Best Feumr Interlocking Nails Guide and Tips?
In the evolving field of orthopedic surgery, Feumr Interlocking Nails have emerged as a vital solution for complex bone fractures. According to a recent study published by the American Academy of Orthopaedic Surgeons, the utilization of interlocking nails can decrease recovery time by up to 40%. This advancement is crucial for improving patient outcomes and reducing hospital stays.
However, challenges remain. A survey conducted by the Journal of Orthopedic Trauma indicates that nearly 30% of practitioners feel uncertain about optimal installation techniques for Feumr Interlocking Nails. Improper application can lead to complications, making it essential for surgeons to undergo comprehensive training. As we explore the best practices for these innovative devices, addressing the points of confusion and potential pitfalls is paramount.
Enhancing familiarity with Feumr Interlocking Nails can significantly impact patient care. Increased awareness about their benefits, as well as the necessary operative skills, can lead to better clinical decisions. Surgeons must engage in reflective practices, continually assessing their techniques to optimize the use of these critical surgical tools.
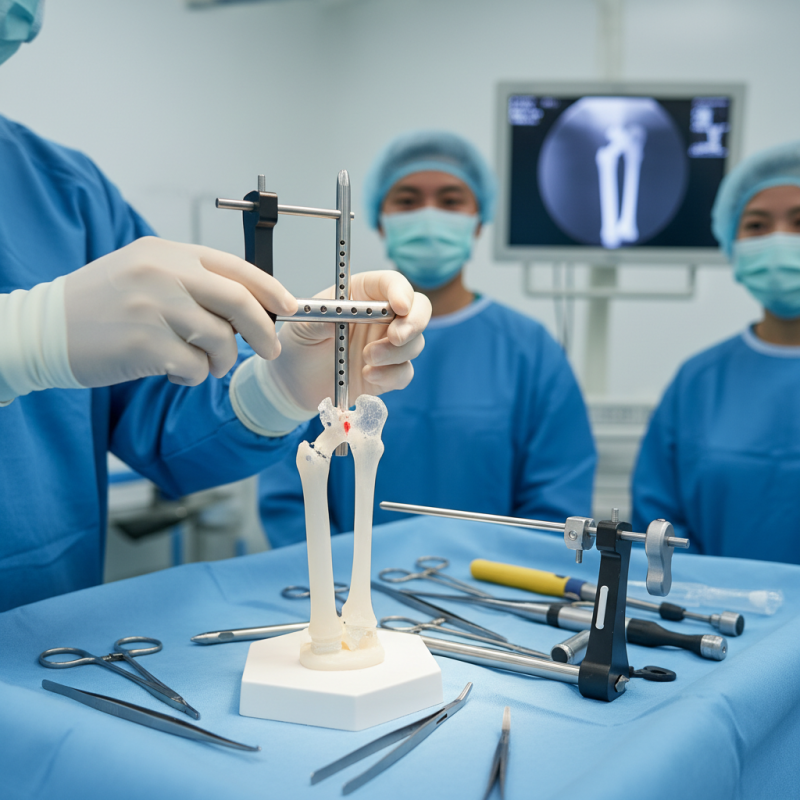
Overview of Interlocking Nails and Their Benefits
Interlocking nails are gaining popularity in orthopedic surgery. They offer stable fixation for long bone fractures, enabling quicker recovery. A report from the Journal of Orthopaedic Trauma states that interlocking nails can reduce healing time by 30%.
These nails are designed to prevent rotational and axial instability. As a result, they enhance the alignment of fractured bones. This is important, especially in complex fractures where traditional methods may fall short. A study highlights that 85% of patients with interlocking nails reported excellent functional recovery. However, not all cases achieve such success.
Using interlocking nails requires careful consideration. Not every patient is suited for this method. Complications may arise, including infection and malalignment. Surgeons must assess the unique needs of each patient. Data shows that while interlocking nails can significantly advance recovery, improper application can lead to setbacks. Awareness of these potential issues is crucial for optimal outcomes.
Types of Interlocking Nails and Their Applications
Interlocking nails play a crucial role in orthopedic surgery, particularly for long bone fractures. These devices come in various types, each tailored for specific applications. The most common types include standard interlocking nails, retrograde nails, and antegrade nails. Standard nails are ideal for diaphyseal fractures. They provide stability and allow for early mobilization.
Retrograde interlocking nails are used for specific cases like femur fractures, where entry is from the distal side. This technique can be challenging, and the orientation must be accurate. Mistakes in placement can lead to complications. Antegrade nails are inserted from the proximal side, often used for more complex fractures. Their versatility allows for better alignment in certain situations.
Surgeons must consider patient factors when choosing the type of nail. Anatomy, age, and activity level can influence decision-making. In some cases, the choice may not lead to the best outcome. Reflection on past experiences is essential. Understanding the limitations of each type helps refine techniques. Ultimately, selecting the right interlocking nail is critical for successful recovery.
Step-by-Step Guide to the Interlocking Nail Insertion Process
In recent years, interlocking nails have gained popularity in orthopedic surgery for their effectiveness in treating fractures. The interlocking nail insertion process requires precision and expertise. Surgeons must assess the fracture type and plan the insertion technique accordingly. Accurate alignment is crucial during insertion to ensure optimal healing.
The insertion begins with the appropriate incision. A guide pin is placed through the nail into the medullary canal. Careful attention to the angle of insertion can affect outcomes. Data shows that successful placements often have a deviation of less than 5 degrees from the intended trajectory. After securing the guide pin, the nail is reamed and slid in place. This step is vital as improper reaming can compromise bone integrity.
Tips for a successful insertion include confirming the nail length before surgery to reduce complications. Keeping the surgical site clean minimizes infection risks. Surgeons should also review anatomical variations carefully. Reflecting on past cases, some experienced surgeons note that patient variability can lead to unexpected challenges. Continuous learning from these experiences is essential for improving techniques and outcomes.
Aftercare and Recovery Tips Following Interlocking Nail Surgery
After interlocking nail surgery, aftercare is crucial for optimal recovery. You will need to keep the incision clean and dry. Change dressings regularly to prevent infection. Watch for signs of swelling or unusual pain. Your body is healing, and each day may be different.
Physical therapy will help regain strength and mobility. Start with gentle exercises as advised by your healthcare provider. Don’t rush the process; it takes time. Listen to your body. Some days will be tougher than others. Make notes about what feels right or wrong. This reflection can guide your recovery journey. Remember, progress is not always linear.
Recovery Outcomes After Interlocking Nail Surgery
Common Complications and How to Address Them in Patients
Interlocking nails are commonly used in orthopedic surgery to treat various fractures. However, complications may arise during the healing process. Addressing these issues early is crucial for a successful recovery.
Infection is one of the most common complications. Signs include redness, swelling, and increased pain. If these occur, it’s essential to consult a healthcare provider quickly. They may prescribe antibiotics to manage the infection effectively. Maintaining proper hygiene at the surgical site can significantly reduce the risk.
Another concern is nail migration. This happens when the nail shifts from its intended position. Patients should monitor their symptoms closely. Unusual pain or loss of function could indicate a problem. If noticed, seeking professional help is vital. Regular follow-ups can help prevent long-term issues.
To promote healing, patients should follow their surgeon's advice regarding weight-bearing and physical therapy. Gradual rehabilitation can facilitate better outcomes. Remember, patience is key. Healing takes time, and so does getting back to normal activities.